Diabetes Reversal Is Real, and Your Body Can Do It Faster Than You Thin
Most people hear the word “diabetes” and immediately think of a lifetime sentence. Daily medication. Constant monitoring. A slow, grinding battle against a disease that only gets worse with time. But what if that story is wrong?
What if the condition affecting more than 830 million people worldwide could be undone, not over a decade of suffering, but in a matter of months, weeks, or even days? What if the body already knows how to fix itself and just needs the right conditions to do it?
Medical science is rewriting the diabetes playbook. And the answers are simpler, faster, and more accessible than most people realize.
A Disease Hiding in Plain Sight
Here is the uncomfortable truth about type 2 diabetes. It is everywhere, and most of the people heading toward it have no idea. One in 10 Americans currently lives with diabetes, and 91 percent of all global diabetes cases fall into the type 2 category. Unlike type 1, which usually appears in childhood and stems from an autoimmune response, type 2 tends to develop in adulthood and is driven by how the body processes food, stores fat, and responds to insulin.
Even more alarming, roughly a third of Americans have prediabetes, a warning stage where blood sugar runs higher than normal but hasn’t yet crossed the diagnostic line. More than 80 percent of those people don’t know they have it.
Dr. Osama Hamdy, senior staff physician at the Joslin Diabetes Center in Massachusetts, compares the disease to termites in a house. You don’t see the damage at first. Everything looks fine on the surface. But behind the walls, something is quietly eating away at the structure. By the time symptoms become obvious, serious internal harm may already be done. That silent damage is exactly what makes type 2 diabetes so dangerous, and exactly why catching it early changes everything.
What Actually Breaks Down Inside Your Body
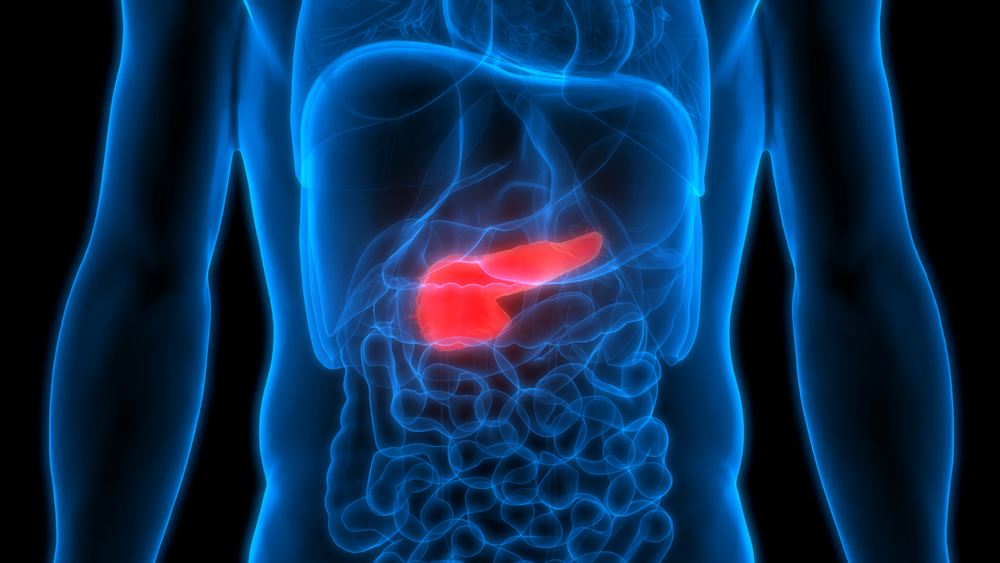
Every time you eat, your digestive system converts food into glucose, a form of sugar that enters your bloodstream. Your pancreas responds by releasing insulin, a hormone that acts like a key, opening the doors of your cells so glucose can enter and provide energy. In a healthy body, the system runs smoothly. Glucose enters cells. Blood sugar levels stay balanced. Organs get the nutrients they need.
In type 2 diabetes, that system fails. Either your cells stop responding properly to insulin, a condition known as insulin resistance, or your pancreas can no longer produce enough insulin to keep up with demand. Sometimes both happen at once.
When glucose can’t enter cells, it builds up in the bloodstream. Over time, that excess sugar becomes toxic. It damages blood vessels throughout the body, and those damaged vessels lead to a devastating chain of consequences.
Diabetes is the leading cause of amputations, blindness, kidney failure requiring dialysis, and a major driver of heart attacks, strokes, dementia, nerve damage, and several types of cancer. Dr. Elizabeth Vaughan, an associate professor at the University of Texas Medical Branch who has co-authored diabetes research, points to damaged blood vessels as the common thread connecting all of these outcomes.
But here is where the story turns. According to Dr. Dariush Mozaffarian, a cardiologist and director of the Food is Medicine Institute at Tufts University, type 2 diabetes is driven by metabolic abnormalities that are largely reversible. Modest weight reduction, a better diet, more movement, and lower stress can restore normal function to the body’s organs and tissues. Your body wants to heal. It just needs you to remove what’s blocking it.
Visceral Fat Is the Real Villain

If type 2 diabetes has a primary antagonist, it lives deep inside your abdomen. Visceral fat, the internal fat that wraps around organs like the liver and intestines, plays a direct role in triggering insulin resistance. Unlike the fat you can pinch on your arms or thighs, visceral fat is hidden. You can’t see it in a mirror, but you can often spot its presence in a protruding belly.
Dr. O. Kenrik Duru, a professor of medicine at UCLA’s David Geffen School of Medicine, explains that visceral fat communicates with the organs responsible for absorbing glucose from the blood. Something about that communication causes those organs to develop insulin resistance, which then sets type 2 diabetes in motion. Scientists don’t yet fully understand the exact mechanism, but the link between visceral fat and insulin resistance is well-documented.
And here is the encouraging part. You don’t need to lose an extraordinary amount of weight to see results. According to Hamdy, even a 7 percent reduction in body weight can improve insulin sensitivity by 57 percent. For someone weighing 200 pounds, that’s just 14 pounds. Not an impossible mountain to climb. A very real, very achievable hill.
Move Your Body, Move Your Blood Sugar

Exercise attacks diabetes from two directions at once. It promotes weight loss, which reduces visceral fat. And it also strengthens muscles so they become better at pulling glucose out of the bloodstream on their own.
Vaughan recommends one of the simplest habits imaginable. Go for a walk after eating. Post-meal movement helps your muscles absorb the glucose spike that follows food, reducing the load on your insulin system when it matters most.
For longer-term results, the American Diabetes Association recommends at least 2.5 hours of moderate physical activity per week, or half that amount in vigorous exercise, plus strength training at least twice a week. Strength training matters because larger, stronger muscles consume more glucose, turning your body into a more efficient blood-sugar-processing machine around the clock.
You don’t need a gym membership or a personal trainer to hit those numbers. Walking, cycling, swimming, bodyweight exercises at home, and even gardening at a brisk pace all count. Consistency matters more than intensity.
Eat Like Your Pancreas Depends on It
Because it does. Diet changes can improve glucose levels by reducing blood sugar spikes and slowing digestion. And the adjustments don’t require a nutrition degree.
Start by cutting refined grains. White bread, white rice, and white pasta all break down quickly into glucose, sending blood sugar levels surging. Swap them for whole-grain alternatives that digest more slowly and release energy more steadily.
Next, eliminate added sugars. Hamdy is blunt on the matter. Added sugars carry no nutritional value and rank high on the glycemic index, making them one of the worst offenders for blood sugar control. Other high-glycemic foods worth limiting include tortillas, crackers, noodles, certain breakfast cereals, and starchy vegetables like corn and potatoes.
On the other side of the plate, increase your fiber and protein intake. Fiber slows glucose absorption and helps you feel full longer. Protein builds lean muscle mass, which in turn improves your body’s ability to process blood sugar. Choose minimally processed foods and lean meats. And drink at least eight glasses of water daily, as water helps your kidneys filter excess sugar from the blood.
None of these changes requires exotic ingredients or complicated meal plans. Simple swaps, repeated daily, create the metabolic environment your body needs to recover.
Sleep and Stress Are Silent Saboteurs

Most conversations about diabetes focus on food and exercise. Few people talk about the two lifestyle factors that can quietly undo all that hard work.
Poor sleep raises blood sugar levels. So does chronic stress. When your body doesn’t rest enough or stays locked in a fight-or-flight state for too long, hormones like cortisol flood your system and push glucose levels higher, regardless of what you ate for dinner.
Vaughan recommends aiming for 7 to 9 hours of sleep each night and building relaxation techniques into your daily routine, whether that means meditation, deep breathing, journaling, or simply stepping outside for 10 minutes of quiet.
Dr. Sun Kim, an endocrinologist at Stanford University who specializes in treating diabetes, reinforces that a combined approach, one that tackles weight, diet, exercise, sleep, and stress together, produces the strongest outcomes. No single change works as well in isolation as all of them work in concert.
So How Fast Can Reversal Actually Happen?
Here is where the story gets exciting. At the Joslin Diabetes Center, Hamdy and his team built a program specifically designed for diabetes remission. Among patients admitted to that program, 80 percent reach remission within two years. Two years might sound like a long time. But for many people, the turnaround happens much faster.
Once excess weight comes off, remission-level glucose numbers can appear within days or weeks. Hamdy compares it to what happens after bariatric surgery, where patients often see blood sugar normalize almost immediately after the procedure. Weight loss through lifestyle changes can produce the same metabolic shift.
Dietary changes alone can also move the needle at remarkable speed. Dr. Kim notes that a person recently diagnosed with type 2 diabetes can bring blood sugar back to normal rapidly, especially if they cut out a major offender. Someone drinking six regular sodas a day, for example, might see dramatic improvement just by stopping that single habit.
But speed comes with a caveat. Remission has a specific medical definition. Your glucose numbers must stay below the diabetes diagnosis threshold for at least three months without any diabetes medication. Getting to remission-level numbers is the first step. Staying there is what counts.
Reversal Is Not a Finish Line
Remission is real. Remission is achievable. But remission is not permanent by default. Significant weight gain can bring diabetes back. A return to old eating patterns can undo months or years of progress. Your body remembers the metabolic pathways that led to the disease in the first place, and it can slide back down those paths if given the chance.
Think of reversal not as a cure but as an ongoing practice. You earned your way out of the disease through daily choices, and you maintain that freedom through the same daily choices.
Dr. Sydney Blount, an assistant professor of medicine at the University of Nebraska Medical Center, offers a final reminder worth carrying with you. Prevention is the best medicine. If you already have prediabetes or a family history of type 2 diabetes, the same lifestyle changes that reverse the disease can stop it from developing in the first place.
Your body built this problem over years of accumulated habits. It can dismantle it in a fraction of that time. But only if you start. And the best day to start will always be today.
Loading...

