Against All Odds, She Weighed Less Than a Pound and Still Made It Home
Some births announce themselves with joy. Others arrive wrapped in silence and fear, where the air in the room shifts and every person present holds their breath. On November 17, 2025, a baby girl entered the world inside King’s College Hospital in Dubai, UAE, under circumstances that gave her almost no chance of survival. Her name was Talia, and from her very first breath, she was already defying what medicine considered possible.
What happened over the next 129 days would leave doctors, nurses, and her parents forever changed, and would write a new chapter in the history of neonatal care across the UAE.
A Birth No One Expected to Celebrate
World Prematurity Day carries a weight that most people never feel personally. For Talia’s parents, November 17 became something else entirely. Talia arrived at just 22 weeks and 5 days of gestation, more than four months before her due date. She weighed 400 grams, less than a pound, roughly the weight of a small apple.
Her delivery was sudden and complicated. She was born still inside the amniotic sac, looking fragile and small, her features not yet fully formed, her skin so delicate and transparent that even gentle handling carried risk. Within moments, the neonatal team began intubation and advanced breathing support before transferring her to the neonatal intensive care unit (NICU).
At 22 weeks, a baby sits at what doctors call “the edge of viability.” A Stanford University study tracking nearly 11,000 preterm infants born between 2013 and 2018 found that with active treatment, only about 28% of babies born at 22 weeks survive. Talia’s weight made her odds even more uncertain. A decision had to be made fast, and both the medical team and her family chose to fight.
When Every Odd Is Against You
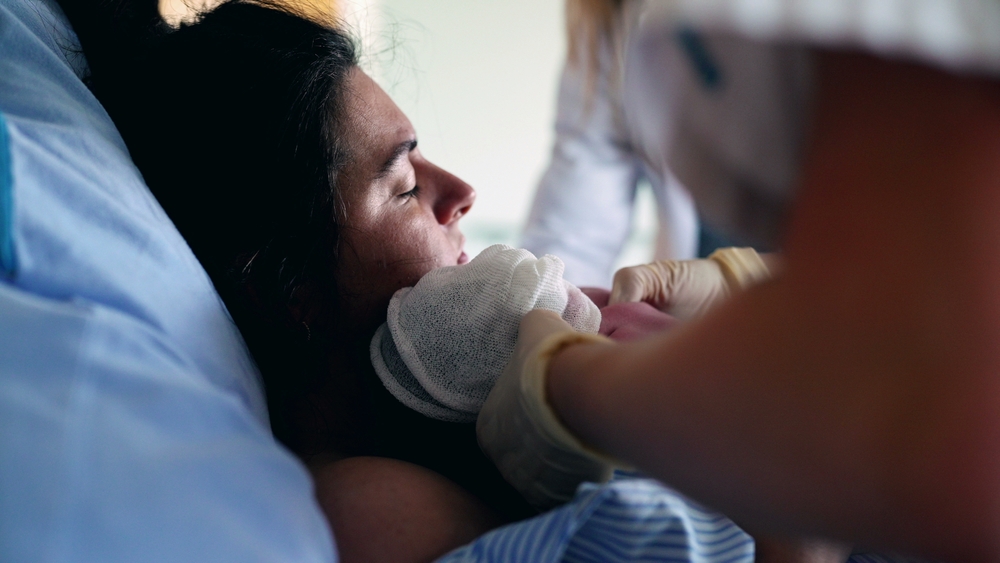
What made Talia’s first hours so precarious went beyond her prematurity. Her mother, Jade Gacera Cubillo, was severely ill at the time of delivery, suffering from serious abdominal and urinary tract infections, and those infections raised her daughter’s risk considerably. Talia showed high infection markers from birth and needed strong antibiotics right away.
Her body was not ready for the world. Her skin offered almost no barrier protection. Standard NICU procedures, manageable with a full-term baby, became extraordinarily difficult given her size. Doctors had to secure vital lines and stabilize her condition in an environment where any wrong move could be irreversible.
Medical teams in neonatal care speak about “the golden hour” in premature births. Every minute in that first window carries enormous consequences. Get it right, and you open a door to survival. Get it wrong, and that door may never open again.
Early brain scans came back with areas flagged for concern, raising the possibility of brain injury from infection and extreme prematurity. Jade and her partner stood by, watching their daughter through the glass, holding onto hope while bracing for news that might shatter it.
129 Days, One Gram at a Time

“This was a baby born at the very limits of what is considered viable. Every step required precision, experience, attention to detail, anticipatory management, and constant reassessment.” Those words belong to Dr. Maria Theresa Reyes, a Consultant Neonatologist at King’s College Hospital Dubai, and they capture something about Talia’s care that statistics alone cannot express.
Day after day, the NICU team responded to each new obstacle. Small amounts of breast milk began helping Talia’s immunity and gut development. Follow-up brain scans brought relief, showing no signs of major brain bleeding. Her condition began to stabilize. She started tolerating feeds. She began to grow.
Weight gain in an extreme preemie is not incidental. Every gram matters, not just as a medical indicator, but as proof that a body too small for the world is learning to belong in it. Over 4.5 months of intensive care, Talia climbed from 400 grams to 2.6 kilograms. She went from requiring machines to breathe to breathing on her own. She went from a baby doctors weren’t sure could survive the night, to a baby ready to go home.
The Team Behind the Record

King’s College Hospital Dubai’s NICU follows UK-aligned clinical protocols and manages some of the most complex and high-risk neonatal cases in the region. To date, its survival rate sits at 99.3%, a number that reflects years of specialized, consultant-led care. Dr. Reyes and her colleague, Dr. Harikumar Nair, led Talia’s case, and both have spoken about how far it pushed the boundaries of what their team had previously seen.
“We have had several 23-week infants weighing around 500 grams with excellent outcomes. Talia is our first 22-week infant, weighing just 400 grams. She is the smallest 22-weeker ever reported in the UAE,” said Dr. Reyes.
That sentence carries more weight than it might first appear. Neonatology in the UAE has grown considerably over the past two decades, with hospitals building specialized units capable of managing increasingly complex cases. Talia’s survival does not just represent one baby’s story. It marks what this level of care can now achieve in a country rapidly expanding its medical capabilities.
What made the difference, according to Dr. Reyes, was a combination of experience, precision, and a team culture built around anticipatory care rather than reactive management. Doctors did not just respond to what Talia’s body was doing. They anticipated what it might do next, and prepared for it.
What Science Has Learned About Saving the Tiniest Lives

Talia’s survival did not happen in a vacuum. It sits on decades of medical research and hard-won knowledge about how to keep extremely premature babies alive and help them grow.
A Stanford Medicine study published in the Journal of the American Medical Association tracked 10,877 premature infants born between 2013 and 2018. Survival rates for babies born between 22 and 28 weeks rose from 76% to 78% compared to the prior period. While two percentage points may sound modest, it represents hundreds of additional infants saved each year.
Key advances have driven this progress. Surfactant therapy, a treatment using a mixture of protein and fat, helps underdeveloped lungs function more efficiently. Prenatal steroids, given to mothers before extremely early delivery, help the baby’s lungs and organs mature before birth. CPAP devices, which keep airways open without the lung damage that mechanical ventilators can cause, have become preferred in many NICUs. Womb-like environments, with low lighting and minimal noise, reduce stress on fragile newborns and support better neurological development.
Kangaroo care, or skin-to-skin contact between parent and baby, has also proven far more powerful than it might seem. Research has shown that it increases weight gain, reduces the risk of sepsis, and improves both survival rates and neurodevelopmental outcomes. At Stanford, teams use neuromonitoring devices to track brain activity and oxygen levels in real time, to minimize brain injury during the most vulnerable period of a newborn’s life.
Even with all these advances, researchers remain focused on what comes after the NICU. Families need sustained support long after discharge, and outcomes matter across a child’s entire life, not just within the hospital walls.
A Mother’s Words, Unfiltered
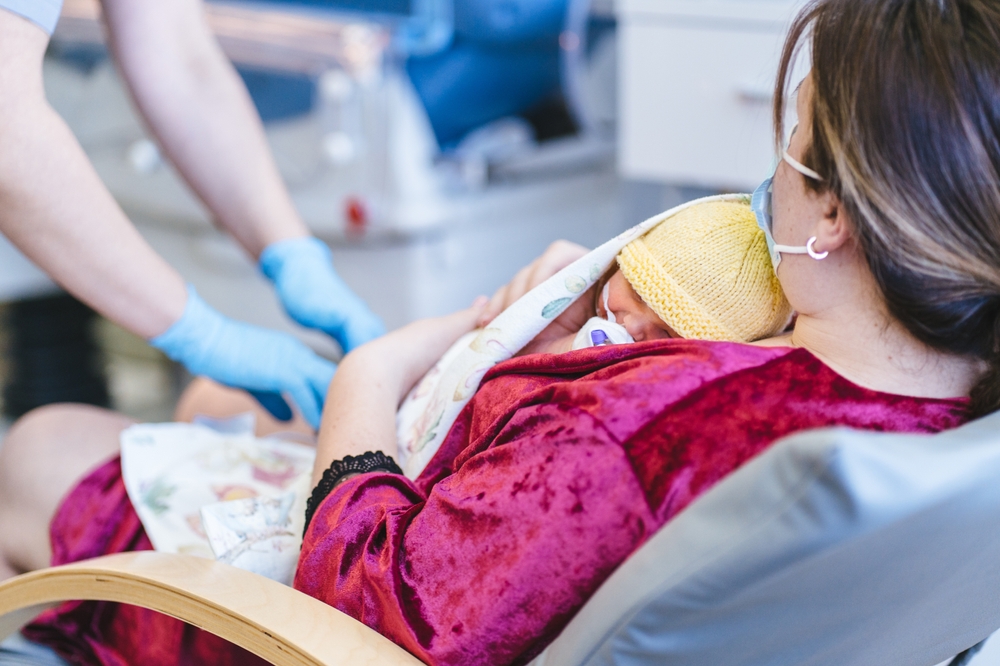
Numbers and medical achievements can only say so much. Jade spent four months standing beside her daughter’s incubator, watching monitors, learning the rhythm of alarms, and finding ways to hold on.
“We learned how to love through wires, alarms, and uncertainty. How to smile while our hearts were breaking. The NICU changed us completely. By God’s grace, she grew stronger each day until she was finally able to come home. We will always be grateful to the team who stood with us through it all,” she said.
Her words cut through the clinical language and remind us what is actually at stake in every NICU case. Behind every survival rate, every scan result, and every gram of weight gained, there is a family learning to live inside the terror of not knowing. Jade and her partner were not passive bystanders waiting for doctors to save their daughter. They were present, they were prayerful, and the experience changed them in ways that no discharge summary can measure.
Home, and What Comes Next
On April 16, 2026, King’s College Hospital Dubai announced that Talia had gone home. She left with no major long-term complications flagged by doctors, though, like all extremely preterm infants, she will need close monitoring and regular follow-up care as she grows.
Her story does not end at discharge. Extreme preemies face an ongoing journey, one that includes watching for developmental delays, supporting lung health, and giving a body that entered the world too early the time and space it needs to catch up. Families in this position need more than medical appointments. They need community, information, and systems of care built to meet them where they are.
What Talia’s story makes clear is that medicine has crossed a threshold. Babies born at 22 weeks now have a fighting chance, given the right care, in the right hands, at the right time. What Dr. Reyes and her team did for Talia goes beyond technical skill. It reflects a belief that even the smallest life, born at the very edge of what science considers possible, deserves every resource and every ounce of effort a medical team can give.
Talia came home at 2.6 kilograms, surrounded by love, carried by faith, and kept alive by science. She will grow up, perhaps never knowing how many people fought for her before she could fight for herself. Some births change the room they happen in. Talia’s changed something larger.
Loading...

